Making sense of the pulse and how PPG data from wearables could shape the future of healthcare
If you’ve ever worn a smartwatch or fitness tracker, you’ve probably seen a graph of your heart rate rising during activity and falling when you rest.
Most of these devices use a clever optical technology called photoplethysmography, or PPG for short. It’s a long word for a simple idea: shining light on the skin to track tiny changes in blood flow. PPG is one of the most widely used signals in wearable technology. But beyond showing your heart rate, it holds far more potential and a few important challenges such as for use in healthcare.
What Is PPG?
When your heart beats, blood rushes through your arteries and capillaries. A PPG sensor uses a small LED to shine light (often green or infrared) into the skin and measures how much light is reflected back. Each pulse changes that reflection slightly, creating a wave pattern that mirrors your heartbeat.
From this signal, algorithms can estimate not only heart rate, but also things like:
Heart rate variability (HRV) how much your heart rate naturally fluctuates, linked to stress, sleep, and recovery.
Respiratory rate small changes in the pulse waveform that correspond to breathing.
Blood oxygen saturation (SpO₂) by using multiple light wavelengths.
Circulatory changes such as blood vessel tone, temperature, or even dehydration.
That’s a lot of information from a simple light sensor and it’s what makes PPG so appealing for continuous monitoring and therefore for use in healthcare.
How Clinicians Might Use PPG Data
Monitoring long-term trends
PPG allows continuous, non-invasive monitoring. Instead of relying on one-off clinic readings, clinicians could review weeks of resting heart rate or HRV data to spot early signs of deterioration or recovery, for example, in cardiac rehabilitation or chronic illness management.Detecting arrhythmias or irregular heart patterns
PPG-based devices have already shown potential to flag possible atrial fibrillation.
While not a diagnostic tool on its own, it can alert clinicians or patients to seek confirmatory ECG testing sooner.Understanding stress, fatigue or sleep patterns
HRV and pulse amplitude variation reflect how the body’s nervous system responds to stress and rest. When combined with sleep or activity data, this can give a richer picture of a person’s overall wellbeing which is valuable in both clinical and occupational health settings.Supporting remote care
For patients recovering at home, continuous monitoring of pulse rate and oxygen levels could help clinicians intervene earlier if a problem develops, without needing a hospital visit, keeping care closer to home.Allowing healthcare staff to understand how a patient’s vital signs operate in the real world. Taking data and reviewing it in a consultation and using the data often alongside other metrics to determine a course of action for the treatment and management of a patient.
The Challenges We Still Need to Solve
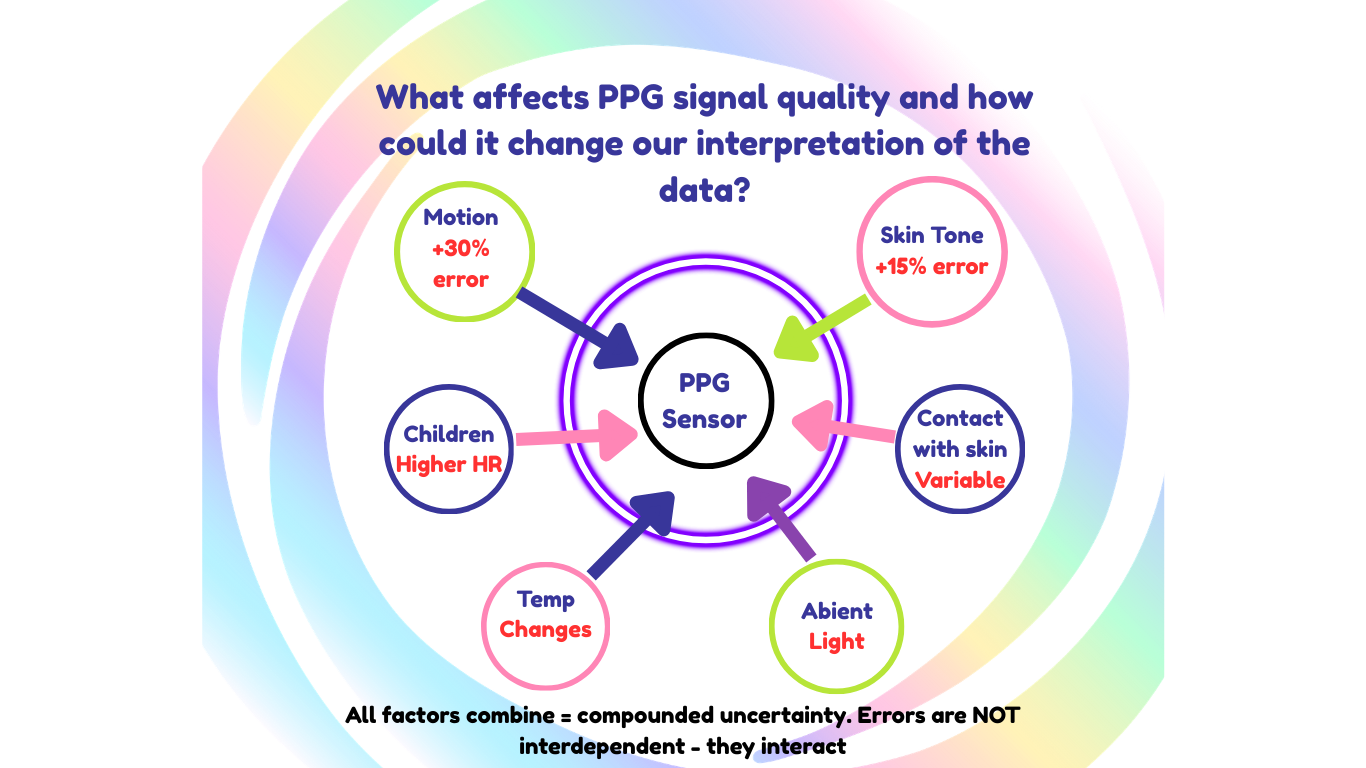
PPG is powerful — but it’s not perfect. Light signals can be affected by movement, skin tone, temperature, contact pressure, and even where on the body the sensor is placed.
Algorithms do their best to clean up the data, but errors still happen, especially when people are active.
This means that not all PPG data are clinically reliable, and not all devices report how confident they are in each measurement. In other words, a reading might look precise, but the uncertainty behind it is often hidden.
For clinical use, that uncertainty needs to be visible and quantified, for example, by showing signal quality scores or confidence ranges. Without that, a clinician can’t easily tell whether a sudden heart-rate change is real or just an artefact.
Building Trust in PPG-Based Wearables
To make PPG data truly useful in healthcare, we’ll need to:
Validate devices across diverse groups (different skin tones, ages, and conditions).
Provide transparency about signal quality and processing methods.
Integrate data safely into health records or remote monitoring platforms.
Educate clinicians about how to interpret wearable data and their limits.
These steps are already reflected in UK policy, including the NHS’s Medium-Term Planning Framework (2025–2029) and Fit for the Future: 10-Year Health Plan, both of which highlight wearables and remote monitoring as key enablers of preventive and community-based care.